When the COVID-19 pandemic tore through towns and cities across the globe, long-term care facilities, which provide care for many people most at risk of severe illness or death due to the virus–the elderly and chronically ill people and people living with disabilities–were hit hard. Outbreaks in these facilities had severe results, with some of the highest infection rates and death tolls among workers and residents. Governments, civil society, unions and watchdog organizations dug in to better understand why long-term care facilities were so heavily unprepared for the pandemic, and many reports pointed to the increased privatization in the long-term care sector heavily driven by private investors and private equity funds.
The effects of privatization of healthcare services have been widely criticized. In countries around the world, evidence is demonstrating that decades of increasing privatization of health has led to services that are of poorer quality, more expensive, and overall less accessible. Most often, the effects of privatization are unjustly felt by poor and marginalized populations who already struggle to access healthcare. During the COVID-19 pandemic, this was tragically seen in long-term care facilities.
Unjust impact of COVID-19 in long-term care facilities
The deaths associated with long-term care facilities, especially in higher income countries, have been staggering as compared to the general population. In Canada, for example, a country where long-term care was particularly badly hit, deaths in long-term care accounted for 79% of all COVID-19 deaths during the first wave, and 60% of all COVID-19 deaths during the second. In the U.S., residents and staff of long-term care facilities made up at least 23% of all COVID-19 deaths as of January 30, 2022.
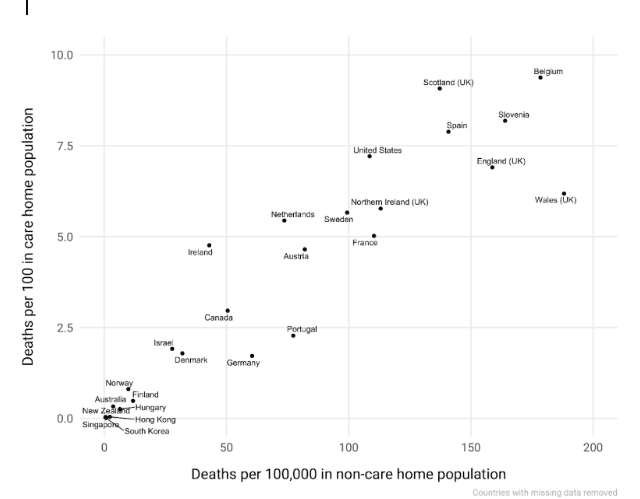
Box: Total number of deaths linked to COVID-19 in the population living in the community, compared to the number of deaths among care home residents (February 1, 2021)
Staff of long-term care facilities, as well as home health care workers, working at the frontlines of the COVID-19 pandemic were at increased risk of exposure to COVID-19 due to the nature of their work. Employers proved to be inadequately prepared for the pandemic and failed to provide adequate protection (PPE) for workers. There was a scarcity of workers as so many became ill with COVID-19, compounded by the longstanding precarity of long-term care workers who often work multiple jobs to make a living wage. In combination with inadequate access to training and support such as sick leave, the shortage of workers further fueled outbreaks.
As governments failed to protect residents and workers and prevent such devastating outcomes in long-term care facilities, the world looked on in disbelief demanding answers as to why this was happening.
Private investment and worsening conditions
The crisis that COVID-19 caused demonstrated how long-term care has been undermined and neglected for decades.
Increasingly, long-term care facilities have moved from public to private operation and ownership. With this has come a re-prioritization of their purpose, where earning profits competes with providing quality care for residents. In a report on long-term care and COVID-19, the European Public Services Union (EPSU) noted that for-profit long-term care facilities experienced higher odds of infection and outbreak than publicly-run facilities. Other risk factors for COVID-19 exposure that the report listed, such as understaffing, reliance on temporary staff, larger and/or crowded nursing homes, and lack of trade unions, are very often associated with privatization that have been shown to degrade quality and accessibility of other healthcare services. Even in publicly-run long-term care facilities, similar risk factors–implemented as austerity measures–fueled outbreaks.
Long-term care is an attractive option for private companies and private equity funds who aim to earn the highest return on their investment. While governments have contracted services out to private operators in an attempt to improve efficiency, private operators have used that as an opportunity to turn a profit by minimizing the care delivered and services offered. Meanwhile, governments continue to transfer around €218 billion to care home operators every year, with residents or their families paying €65 billion more.
While providing substandard services and maintaining poor working conditions, companies that operate for-profit long-term care facilities have paid out huge sums to their investors. Investigate Europe reported that they also often avoid taxes on this money by moving it to offshore accounts. Ultimately, these companies siphon public money into their own bank accounts while conditions worsen for residents and workers at the long-term care facilities they operate.
Protecting health and dignity must prevail over profits
The issues are not new: the pandemic’s toll could have been mitigated if we, as a society, had better managed the way we collectively arrange care for the elderly, the chronically ill, and people living with disabilities. Disability justice activists even challenge us to question the very model of long-term care.
Rather than rethink long-term care and even healthcare services broadly, governments and companies have worked to deepen privatization and have leaned into a more commercialized approach. This approach has been and continues to be harmful to people’s health and detrimental to the right to health. In response, activists across the globe have mobilized against the profit motive of privatized and commercialized health services, calling for strengthened public health systems that are truly driven by achieving the best health outcomes for everyone.
The wider public must begin questioning private ownership and management of long-term care facilities. We must demand protection of the dignity and the rights of the people who live there, and that the labor of people who work there is valued.
Leigh Kamore Haynes is an organizer with People’s Health Movement networks in Europe and in the USA.
Baijayanta Mukhopadhyay is a family physician and helps coordinate the People’s Health Movement’s Canadian chapter.

