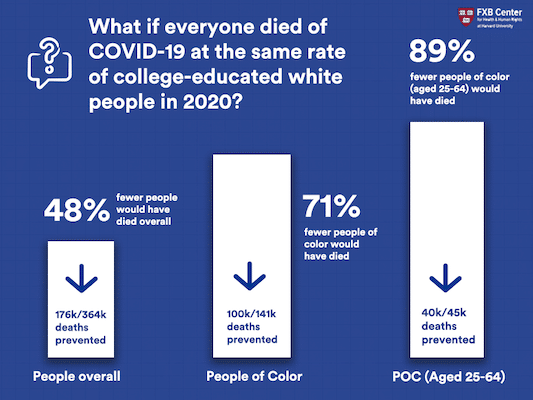
Are you searching for a way to highlight the negative consequences of racism? Try this: Justin M. Feldman and Mary T. Basset, in a recently published study, found that if everyone living in the United States, aged 25 years or older, died of COVID-19 at the same rate as college-educated non-Hispanic white people did in 2020, 48 percent fewer people would have died, 71 percent fewer people of color would have died, and 89 percent fewer people of color aged 25-64 would have died.
The following infographic includes the actual number of lives that could have been saved.
The study
Feldman and Basset used a newly available public data set on COVID-19 mortality—one that allowed them to group the deaths of all persons in the United States, aged 25 years or older, by age, sex, race and ethnicity, and educational attainment—to test 3 hypotheses:
- That “racial and ethnic minority populations would experience higher age-adjusted COVID-19 mortality rates than the non-Hispanic white population.”
- That “within racial and ethnic groups, age-adjusted COVID-19 mortality rates would be highest among those with the lowest educational attainment.”
- That “racial and ethnic inequalities in COVID-19 mortality rates would remain when comparing within levels of educational attainment.”
Finally, as highlighted above, they also estimated the number of deaths that would have occurred if each racial and ethnic population group had “the same cumulative mortality rate as the group that, theoretically, has the most racialized socioeconomic privilege: college-educated non-Hispanic white individuals. We did this by multiplying each stratum’s populations size by the mortality rate observed among college-educated non-Hispanic white individuals of the same age and sex.”
Results
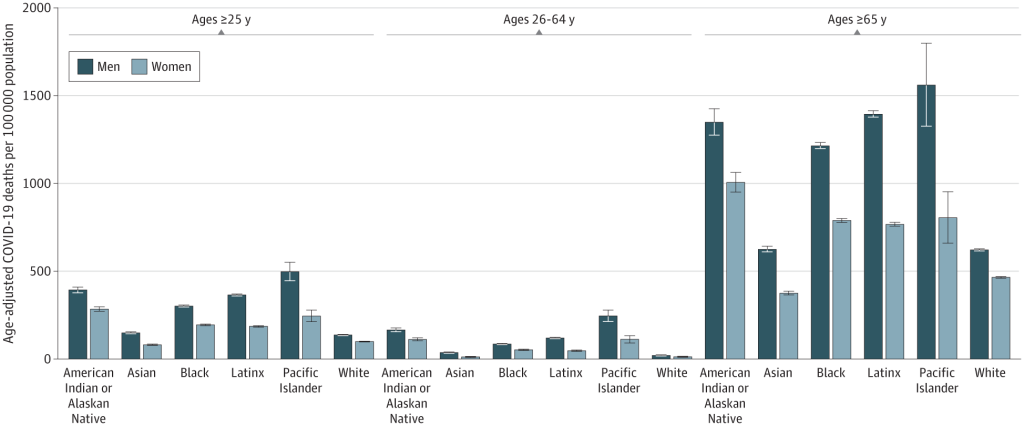
The results of their first hypothesis test—to determine whether racial and ethnic minority populations experience higher age-adjusted COVID-19 mortality rates than non-Hispanic whites—are illustrated in the figure below. As we can see, in each of the three age groupings, racial and ethnic minorities, with the exception of the Asian population, experienced significantly higher mortality rates than non-Hispanic whites.
For those aged 25 and over, the cumulative 2020 mortality rate per 100,000 population was:
- 334.5 for American Indian or Alaska Native
- 110.9 for Asian
- 237.9 for Black
- 265.2 for Latinx or Hispanic
- 356.9 for Hawaiian and Other Pacific Islander
- 116.4 for white
Not only did all the racial and ethnic populations, with the exception of Asians, experience far higher COVID-19 mortality rates than did whites, their respective rates were at least twice that of whites.
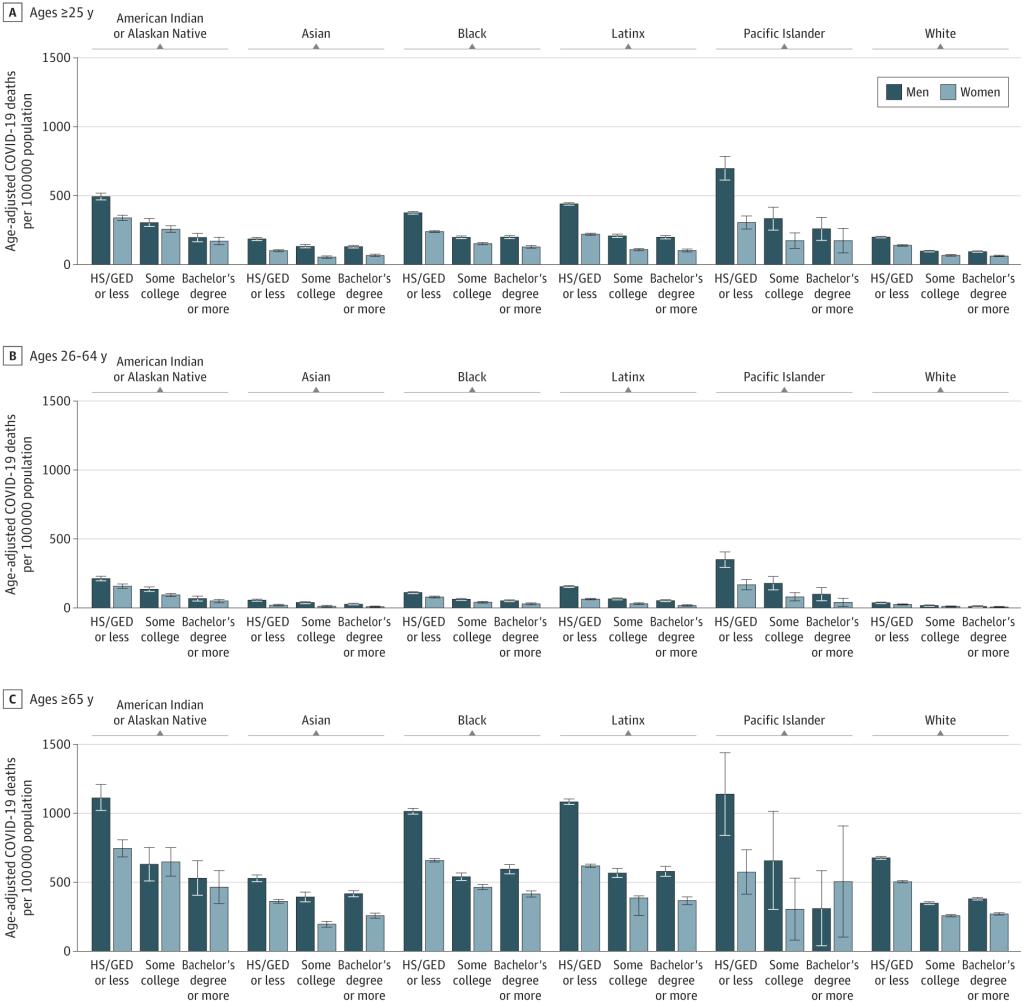
The results of their second hypothesis test—to determine whether for all population groups, age-adjusted COVID-19 mortality rates were highest for those with the least formal education—are shown in the following figures. And as we can see, the highest age-adjusted mortality rates were in fact experienced by those with no college experience.
At the same time, looking across populations, we can again see the destructive impact of racism. For those aged 25 or older, white men with the least education died at a rate of 199.7 per 100,000 population. This was roughly the same as the mortality rates of college-educated non-Hispanic Black men (199.4 per 100,000 population), college-educated American Indian or Alaska Native men (196.3 per 100,000 population), and college-educated Latino men (198.6 per 100,000 population), and significantly lower than that of college-educated Native Hawaiian and Other Pacific Islander men (259.6 per 100,000 population).
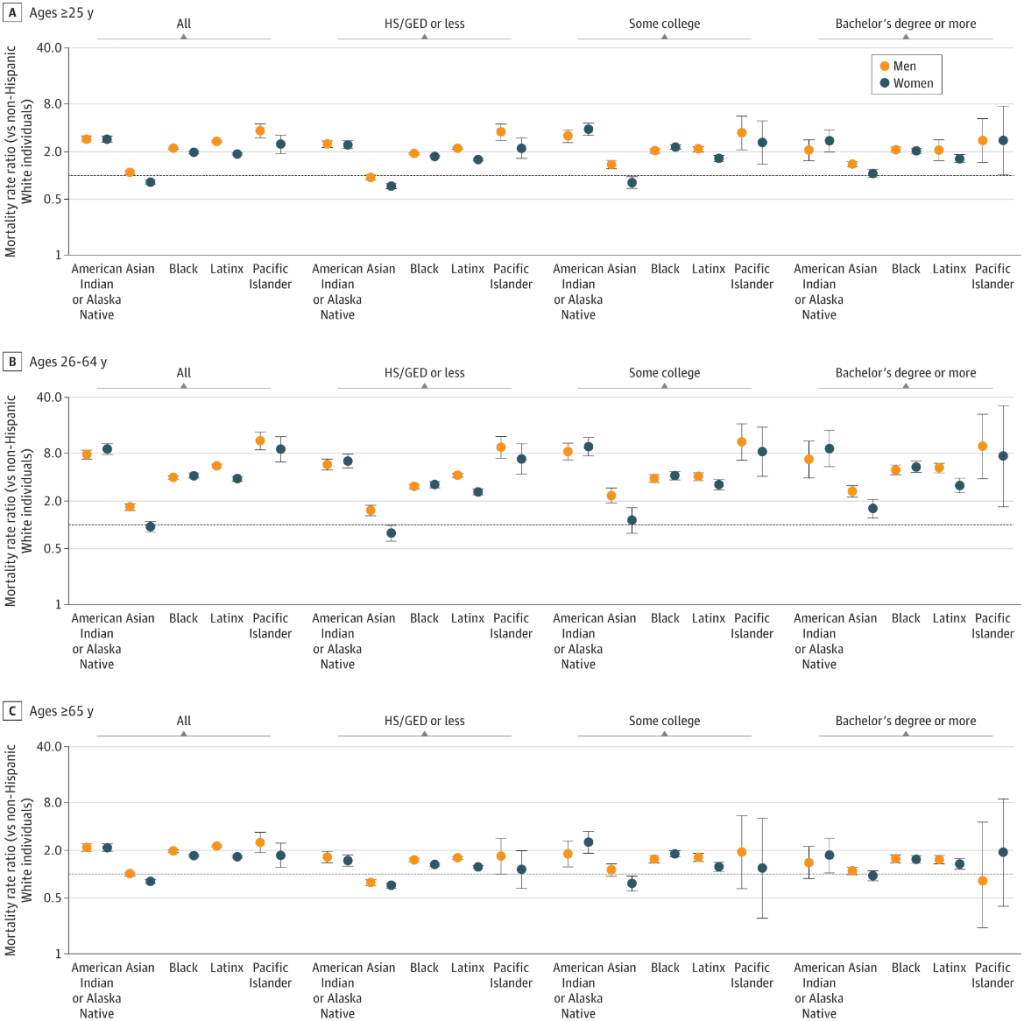
The results of their third hypothesis test—to determine whether racial and ethnic inequalities in COVID-19 mortality rates remain even after adjustment for educational levels—are illustrated in the figures below. The black horizontal line at 1.0 represents the mortality rate of non-Hispanic whites, with the error bars showing 95 percent confidence intervals. A mortality rate ratio of greater than one means that a racial or ethnic subgroup has a higher mortality rate than the educational equivalent non-Hispanic white subgroup.
As we can see, almost all subgroups (54 of 60 age-sex-race-education subgroups, with ages either 26-64 or 65 and over) experienced higher mortality rates than their non-Hispanic white counterparts. “The only groups with lower mortality than non-Hispanic white individuals were: older Asian women of all 3 education levels, younger Asian women in the lowest education category, older Asian men in the highest education category, and older Native Hawaiian and Other Pacific Islander men in the highest education category.”
The results for those 26-64 years of age are especially striking. Despite adjusting for educational attainment, most racial and ethnic subgroups experienced mortality rates two to eight times greater than their white counterparts. This extreme divergence in COVID-19 mortality rates can only be understood in light of the country’s long history of racially motivated policies and the resulting extreme differences between most whites and people of color in earnings, wealth, quality of housing, access to health care, and conditions of employment.
The size of this divergence does not mean that we should dismiss the challenges facing many non-Hispanic whites. Their mortality rates are no gold standard. Tragically, however, the racism that underpins this divergence also continues to be a major driver of white support for politicians who oppose policies that could help reduce mortality rates and improve living and working conditions for most workers, like the establishment of a single-payer healthcare system. The cost of racism remains extremely high in this country.