On March 16, the prime minister of the Netherlands, Mark Rutte, gave a televised speech to the nation in which he stated: “[We] can delay the spread of the virus and at the same time build up population immunity in a controlled manner.” He went on to say that “[The] bigger the group that acquires immunity, the smaller the chance that the virus can make the leap to vulnerable older people or people with underlying health issues” and added that
We have to realize that it can take months or even longer to build up group immunity, and during that time we need to shield people at greater risk as much as possible.
This idea of letting the population build up immunity by forgoing a complete lockdown and allowing a limited number of infections to take place in low-risk groups—sometimes termed a “stop-and-start COVID quarantine”—has been taken up by such prestigious publications as Science and The New Yorker, among others. It is an idea that seems to be catching on in the United States, tied in as it is to the frantic push by the Trump administration and some Republican governors in states like Georgia, South Carolina, Mississippi, and Florida to re-start the economy and get back to so-called “normal” as soon as possible.
While superficially appealing, this idea of letting some of the population intentionally get infected with the novel coronavirus means that you are implicitly accepting the fact that people will needlessly die due to this policy. It also rests on three inter-related assumptions: first, that one could even relax mitigation measures with COVID-19; second, that there is a robust testing and contact-tracing program already in place; and, third, that if a cluster of COVID-19 cases should break out, it will be rapidly detected and contained.
But do these assumptions hold up to the test? To find out, we must first take a quick look at some recent history.
A short backgrounder on relaxed mitigation. In late December 2019, a novel SARS-like coronavirus originated in Wuhan, China. That country reported its first 41 cases to the World Health Organization on December 31, 2019, although many observers believe that this outbreak actually began much earlier. Since January 2020 to the present, this novel coronavirus—named COVID-19—has spread to 208 countries and territories, and two cruise ships. As of April 22, there have been 2,665,122 reported cases worldwide, with 185,494 deaths. In the United States on that same date, there were 867,771 reported cases with 48,900 deaths—the vast majority in New York City.
These numbers, if anything, are likely an underestimate of the true impact of the COVID-19 pandemic, since death by COVID-19 is not reported as the primary cause of death on standard death certificates in the United States. As the Washington Post noted: “[S]ome people who die at home or in overburdened nursing homes are not being tested, according to funeral directors, medical examiners, and nursing home representatives.” In addition, the tests are not always 100 percent accurate, which means that some people who test negative in fact have the disease. At this time, it is not known how many people are infected with this new coronavirus since routine nationwide testing for infection is not currently performed anywhere in the United States.
The global response to this pandemic has been as varied as the countries infected by it. Responses range from the total lockdown of Northern Italy—which included border closures and bans on the entry of most travelers from other countries—to the Netherlands’ approach of encouraging a social distance of 1.5 meters (just under 5 feet) between persons. The latter country is a heavy promoter of the notion of what it calls an “intelligent” or “targeted” lockdown—an approach which at least one Dutch global health expert characterized as cold and calculated. Under this scheme, only businesses that require close contact—such as hairdressers, beauticians, and massage therapists—are required to cease operations; others can continue to conduct business-as-usual. The stated goal is to not overreact with stringent shelter-in-place requirements. And by keeping things as normal as possible, many healthy people will likely be exposed to COVID-19 and with any luck become immune to it—a process known as “herd immunity.” According to the head of the Netherlands’ National Institute for Health, Jaap van Dissel, since this policy was implemented last month, only 3 percent of the Dutch population have developed antibodies to COVID-19.
But as the BBC pointed out, the problem with this policy is that allowing a killer virus to spread through a community in order to create some level of immunity to a novel disease “implicitly means accepting people will die.” In the United Kingdom, studies revealed that if such an approach were followed there, about 250,000 lives would be lost in that country alone.
Some countries take this laissez-faire idea of herd immunity even further; Sweden is apparently not doing anything to contain COVID-19. Unlike its neighbors Norway and Finland, Sweden has not ordered any lockdowns amid the novel coronavirus pandemic. This means that restaurants and gyms in Sweden are open, there are no border closures or school closings, and life appears largely unchanged—although the government has banned gatherings of over 50 people and encourages people to work from home.
But have the Dutch and Swedish experiments in promoting herd immunity worked?
The answers lie in the numbers.
When the Dutch government implemented this policy back in mid-March, the Netherlands had 278 reported cases (likely an underestimate since most people were not being routinely tested) and 28 deaths due to COVID-19. On April 23, after about one month of this relaxed approach, those numbers had swelled to 35,729 cases and 4,177 deaths, with fewer than 300 recoveries. The Netherlands data is shocking—for a gain of a mere 3 percent herd immunity, they have had an increase of more than 35,500 cases and more than 4,000 deaths. Which makes one wonder if the cost in human cases and deaths was worth the benefit in herd immunity.
As for Sweden’s very relaxed approach to COVID-19, as of April 23, Sweden recorded 16,755 total cases, 2,021 deaths, and 550 recoveries.
Obviously, the goal of “titrating control measures to keep the demand for hospital beds below a maximum capacity”—as the authors of an editorial put it in the peer-reviewed journal Science—hasn’t quite worked out according to plan for the Netherlands and Sweden. A modeling study led by Niall Ferguson of University College London suggested that the only viable option for flattening the curve for the COVID-19 pandemic should include a variety of social distancing measures until a vaccine or antiviral drug becomes available.
Clearly, from looking at the Dutch and Swedish experiences, there is a critical need for nationwide social-distancing measures.
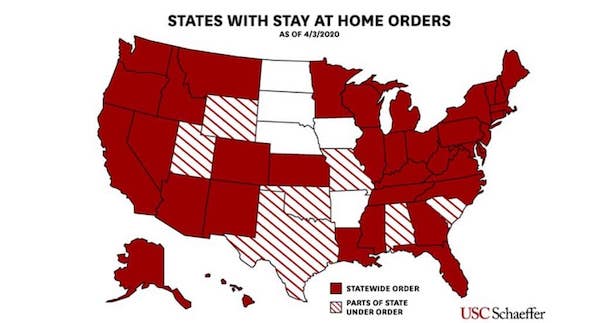
Unfortunately, however, the United States’ response has turned into a crazy quilt of different efforts, ranging from shelter-in-place and stay-at-home orders at the state and local levels of government to states that have no restrictions of any kind. Some states have gone so far as to enact border and road closures for automobiles with out-of-state license plates, while others have no restrictions at all on incoming people and vehicles—jeopardizing not only the health of their residents but the health of visitors to their states. (See Figure 1 above, “States with Stay at Home Orders.”)
Could these mitigation measures be turned off and on like water out of a faucet? Some observers have called social-distancing measures draconian (even though have been used effectively since the time of the Black Death to control pandemics) and argued that they could be relaxed once in a while. Part of their argument is that if case numbers increase, these measures could be quicky and easiliy re-imposed to control the virus, much like turning water off and on from a faucet. If COVID-19 had a reproduction rate (abbreviated as RO) of 1, then this might be a feasible scenario. Yet, based on the epidemiology of this disease and how fast it spreads through populations, it is equally likely that we cannot easily control the virus once mitigation measures are removed and case numbers increase.
Several groups have estimated the RO for the coronavirus to be between 1.5 and 3.5, although there is considerable uncertainty about this range. For illustrative purposes, assuming a RO of 2, the chart below demonstrates how quickly one infected person, either symptomatic or asymptomatic, could go on to infect others. (See figure 2.)
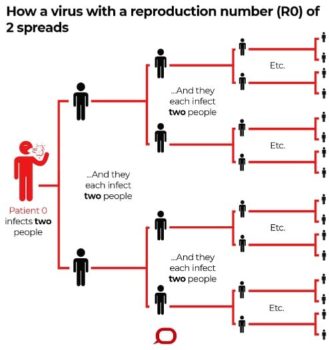
Figure 2. R0 describes how many cases of a disease an infected person will go on to cause—in this imagined scenario, R0=2.
And, once this happens, it may be too late to control a new outbreak of infection. It also assumes one outbreak at a time—which may be magical thinking, given the recent unfortunate experience of countries in Asia, that seemingly had COVID-19 under control but later discovered otherwise.
Testing, testing. In a November 2005 speech at the National Institutes of Health, then-President George W. Bush described how a pandemic would unfold:
A pandemic is a lot like a forest fire… If caught early, it might be extinguished with limited damage. If allowed to smolder, undetected, it can grow to an inferno that can spread quickly beyond our ability to control it.
Given how easily this virus spreads through populations, coupled with the fact that neither the United States nor any other country has yet been fully able to control it, the only interventions we have involve social distancing; testing everyone in order to get a handle on how many people are infected (symptomatic or asymptomatic); finding out where they were infected; isolating the infected from the uninfected; performing rigorous contact tracing; and validating whether current mitigation measures are reducing the population burden of infection.
Some countries, notably Austria and Denmark, are already reopening their countries after coronavirus lockdowns, hoping that they may have already weathered the worst of the first wave of the pandemic. Given the recent experiences of Singapore, Hong Kong, South Korea, and Taiwan—countries which seemed to flatten the curve, only to see the coronavirus bounce back—now may not be the time to relax the mitigation measures that have taken weeks to months for people to accept and adopt. They’re working!
Eileen Choffnes is the immediate past director of the National Academy of Medicine’s Forum on Microbial Threats, a program focused on emerging, reemerging, and novel diseases and the role of human and environmental factors in disease emergence and spread. She has served as a senior scientist with both the Environmental Protection Agency and the Department of Energy. From 1988-93 she served as staff scientist to the Senate Governmental Affairs Committee, working on chemical and biological arms control issues.